Healthcare workers on what it is like to work for Britain’s NHS

Roula Khalaf, Editor of the FT, selects her favourite stories in this weekly newsletter.
It is 75 years since the National Health Service was created and its founding principles — that everyone should have access to healthcare based on an individual’s health needs, not their ability to pay — remain as relevant today as they ever were.
To mark this milestone, the Financial Times asked readers who work for the NHS to share how they feel about the service and tell us about the issues they face in their working lives.
Hundreds of workers, from nurses to junior doctors and GPs to surgeons, shared their views via an FT survey earlier this year. Having worked flat-out during the pandemic, spurred on only by applause, staff told us that they are feeling burned out and disillusioned. They also explained some of the factors driving the continuing strikes by nurses and doctors over pay and conditions.
Some frontline staff who responded to the survey blamed the NHS’s problems on a capacity squeeze that they said reflected a lack of long-term investment and strategic planning. Others said poor IT had prevented attempts to improve efficiency across hospitals. But while opinions on how to fix the NHS differed, there was a shared feeling of pride in the NHS among many of the responses.
A range of views from healthcare workers are published below. Join the conversation by sharing your views in the comment section.
What does the NHS mean to you?

Alison, hospital consultant, 56, says: “If we lose the NHS it would symbolise a lack of regard for the principles on which it was set up: universal, equitable, comprehensive, high quality and free at the point of delivery. It sounds like a cliché but at the heart of the NHS are compassionate, clever, dedicated people who care about their patients and about making a difference. Compared to many health systems, we have incredibly high standards within the NHS with an inherent morality and integrity that puts patients first.”
A female clinical psychologist, 34, says: “People don’t understand what the demise of the NHS actually means. People will need to pay for private care — first, it will be the odd private dentist or GP appointment, but then you’ll need to save thousands for a small operation. And bad luck if you have one of the big illnesses and need A&E or cancer services. It’s going to be a shock for the middle classes if the NHS goes.”
A male consultant, 49, says: “Without the NHS Britain would be an even more unequal place than it already is. Having worked in healthcare systems in countries with very different approaches including Australia, the US and Germany I think the benefits of having a universal national system free for the user are overlooked.
“Of course there are waiting lists, an element of rationing and restrictions to some treatments but this is the case in almost every system for the broad majority of people — unless you are a top earner. Take Germany for example. If you are a member one of the most common health insurance schemes, waiting times for a simple scan or specialist review can take 6-12 months — if you are accepted at all.”
A female psychological therapist, 51, says: “Britain without the NHS would look like dentistry — people will have untreated health problems and those on low incomes will be without adequate healthcare. There are currently many parts of the country where people can’t even access NHS dentistry.”
What issues do you face at work?

Mike, paramedic, 35, says: “It’s impossible to provide adequate patient care. We have to jump-start our ambulance, daily. We don’t have enough equipment to fully kit the ambulances. And I’m exhausted — I work 12-hour shifts and haven’t had a lunch break for about six months.”
Ruth, registrar, 42, says: “We are not able to do our jobs properly and the frustration is palpable and growing. I am a surgical junior, and I am constantly blocked from operating on patients who urgently need emergency surgery because there are no recovery spaces.
“Add to that, the basics just are not there. There are not enough printers to go around so we often have to walk to several different wards to print off a discharge summary. We have exceptionally great staff in our unit, from housekeepers to nurses to consultants, and it’s depressing not being able to do our jobs properly.”
A male nurse, 40, says: “Understaffing is the main one. Lots of people left during the pandemic, and the number of staff who leave within a year of qualifying is rising. We are a highly skilled workforce who make life-saving decisions but we also suffer the indignity of verbal and physical abuse as a ‘normal’ part of the job. We also end up working much longer shifts than we are paid for and work through our breaks all whilst being paid less than we would in most other workplaces.”
Arnoupe, GP, 36, says: “Patients have multiple problems that we cannot always deal with in one appointment. This means that doctors run late or they have to restrict a patient to one problem. Neither option is satisfactory and people get frustrated and angry because of it.”
Robert, consultant, 58, says: “We have had another IT change imposed on us to replace paper with digital files. In principle, this is a good thing but the problem is that the system doesn’t work. Administration work is now being done by senior clinicians, which is taking up precious time that could be spent with patients.”
Terry, emergency medical technician, 35, says: “I have worked for the London ambulance service for more than five years and I believe the service is stretched so far I find it hard to believe it can be saved with this current government. I have personally attended jobs where we have arrived late and the patient has been deceased on arrival. This is unacceptable. I love helping people and assisting those in need, but the role has changed and the NHS needs help and a serious plan moving forward.”
A male consultant in intensive care, 60, says: “I work in a London teaching hospital in an intensive care setting. We are worked off our feet and we are not helped by the incompetence of the management system within the NHS both locally and nationally, as well as the total failure of the current government. I love my job but am feeling totally overwhelmed and frustrated by the current situation.”
A female staff nurse, 51, says: “I am an A&E nurse and we are unable to move patients due to there being no flow in our hospital. We are again nursing patients on our corridors, compromising their privacy and dignity and our working environment.”
What are the problems currently facing the NHS?
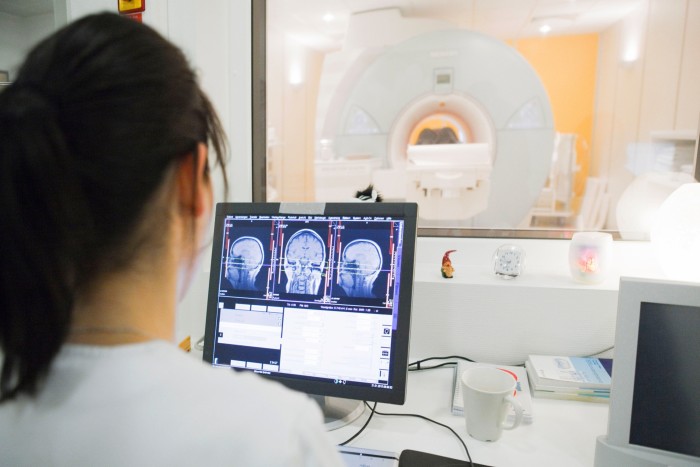
Andrew, retired consultant radiologist, 75, says: “The UK has never trained enough doctors. The NHS has relied on importing staff mostly from South Asia in earlier years and the EU in recent years. This latter supply was abruptly interrupted by Brexit and now the one-off expansion of medical school numbers allowed during the Covid crisis has been reversed back to former numbers. What idiot in the Treasury thought this was good idea?”
David, former consultant in hospital practice, 63, says: “The NHS will always be in the twin states of determined denial and forlorn failure. Beset by incompetent and often inept or cynical local management, dishonest regulators, and vainglorious political masters, the usually brilliant staff have neither the support nor the training and circumstances in which to give their best. But always get the blame.”
Yousef, breast surgeon, 63, says: “GP referrals have almost doubled in the last three years, and yet the team I work with remains the same size.”
Does the NHS have a future?

Lisa, healthcare assistant, 54, says: “The NHS is not broken, it is the external elements that make the NHS look irreparable. The NHS as a whole does need a well-aimed kick up the arse. But the fundamental care for patients is still there. Staff can be overworked, and morale is sometimes at an all-time low, but we pick ourselves up, dust off our uniforms, and keep looking after the patients to the very best of our abilities.”
A male consultant surgeon, 55, says: “The NHS can’t survive in its current form. The inefficiencies are staggering and there simply isn’t the number of frontline staff delivering care. Good managers are essential but there has been a burgeoning of ineffective layers of management which slows important decisions and implementation.
“Love it or loathe it, the private sector hospitals are far more efficient: their management structures are much leaner and there is direct responsibility and accountability which seem to be lacking in the NHS, where poor performance is tolerated across all pay grades and roles.”
Stephen, interim manager of transformation, 74, says: “The NHS needs more money to survive. The government has to stop seeing investment in the NHS as a cash drain, rather than an investment in a healthy workforce. Firstly it would be better if all social care and the NHS worked together; second, acute trusts were given adequate block financial grants (as they were during the pandemic), and third, the Treasury did not take back money at the end of the year that it has given to trusts.”
A female clinical psychologist, 33, says: “Just give clinicians the resources to do their jobs properly and improve their working conditions. We need places to eat on breaks, free coffee/tea, access to talking therapy, free car parking, proper admin staff who can help us, and access to research funding among other things.
“Moving to a private system would take 10 years+ meaning more chaos, and is not a silver bullet. Keep what we have and make it better by treating staff as humans and not as replaceable drones.”
Martin, operating department practitioner, 49, says: “The NHS has survived recently due to staff goodwill and their desire to not let their patients and the health service down. After years of tolerating suboptimal conditions, this goodwill is now broken. To rebuild this goodwill we need to reinvest into the NHS to ensure that we have fit-for-purpose buildings which provide the required capacity and workforce for us to be able to safely and efficiently deliver our service. The current culture is to consolidate services, merging those that are under-resourced into one service, though that one service is still under-resourced, and to encourage staff to just get on with it and make it work. This does not ensure patient safety or professional job satisfaction. Currently, there is poor pay and conditions for much of the NHS staff as we haemorrhage doctors and nurses out of the healthcare system to the private sector and other industries.”
Pragya, female junior doctor, 26, says: “The NHS should be managed independently. It needs someone managing it who has an outlook of more than four years in power — not someone who is just angling to be the next chancellor or PM. Contracts should be given out on merit and value, not Tory cronyism. It desperately needs streamlining and modernising but ultimately it needs to preserve staff.”
Kim, healthcare assistant, 39, says: “We need better communication with the public on what they can/not expect from NHS services. If you don’t want to give up your job to look after your sick family members then you have to pay someone to do it. If you don’t want to pay more taxes then that’s the sacrifice you’ll have to make. It’s brutal but at least it’s honest.”
Michael, consultant, 60, says: “What we need is a change of government. If the public wants the NHS to survive they need to kick the Tories out and put their trust in Keir Starmer and Labour. In my 30 years of working in the NHS the Tories have never taken care of the NHS. If you believe that free healthcare is one of the defining features of a civilised society then we need a change of government.”
Mike, consultant, 55, says: “We must ensure that we fix retention first. We do this by paying people fairly, with pay that keeps up with inflation and comparator professions, the sort of careers that those choosing medicine might [otherwise] consider.”
* Some comments have been amended for brevity and to reflect FT style. A few responses are anonymous in line with the reader’s wishes.
Comments