Polio returns to the US after decline in vaccine uptake

Roula Khalaf, Editor of the FT, selects her favourite stories in this weekly newsletter.
“Polio is spreading in Rockland county. Our new generation is in danger,” warns a poster pasted to the wall of a supermarket in Pearl River, a commuter town on the fringes of suburban New York.
It records the re-emergence of the disease as a public health threat, four decades after US authorities had eliminated its transmission with a nationwide childhood vaccination scheme. Last month, New York state’s governor, Kathy Hochul, had to declare a disaster emergency after the virus was detected in several counties’ wastewater, prompting fears that there could be thousands of asymptomatic infections.
It followed the diagnosis, in July, of the first polio case in the US since 2013 in an unvaccinated man in his twenties, who went to doctors in Rockland with his legs partly paralysed. His infection has since been linked via genetic sequencing with the detection of vaccine-derived polio (VDP) in wastewater in London and several infected children in Israel, although he did not travel abroad during the incubation period.
VDP is an illness that occurs when there is poor vaccination coverage. It is caused by the weakened poliovirus that is contained in the oral polio vaccine, which is given to children in much of the developing world. If this weakened virus is then able to circulate a lot, because of low vaccination rates, it can mutate and lead to VDP, which sometimes causes paralysis. In most of the developed world, including the US, an injectable vaccine containing inactivated poliovirus is given, which does not carry the risk of mutation.
Experts say the VDP cases in rich countries — alongside recent outbreaks of wild polio in Afghanistan, Pakistan, Malawi and Mozambique — show how the virus is exploiting disruption to inoculation programmes caused by Covid-19, rising vaccine hesitancy, war, and climate-related disasters. They warn this is a wake-up call for health authorities, which initiated a global campaign in 1988 to eradicate a disease that can kill and disable children.
“As long as polio is anywhere in the world, it poses a threat everywhere — especially with international travel picking up again,” says Carol Pandak, director of Rotary International’s PolioPlus program, which is part of an organisation spearheading the Global Polio Eradication Initiative.
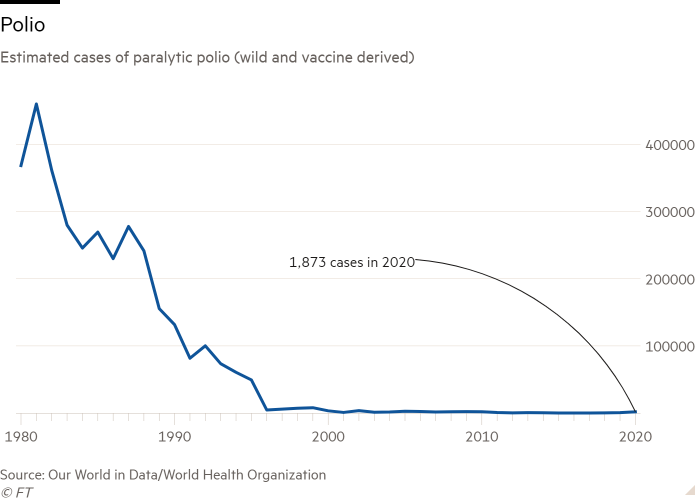
Gpei, which was founded in 1988 through a World Health Assembly resolution, targeted eradication of polio by 2000 through a global childhood immunisation campaign, financed by the public and private sectors. It failed to meet that ambitious goal but, by spending about $19bn on buying and distributing 2.5bn vaccines, the initiative has slashed the number of polio cases by 99.9 per cent and saved an estimated 20mn children from paralysis.
Gpei’s work has helped eradicate two of the three wild poliovirus strains in the past decade. And the virus is now endemic in only two countries — Afghanistan and Pakistan — compared with 125 when its vaccination campaign began.
Yet experts now warn this progress could be squandered unless governments and donors can find an extra $4.8bn to fund a five-year plan for boosting vaccination rates, which have been flagging following the pandemic.
Some 7mn more children missed their third dose of polio vaccine last year, compared with the pre-pandemic year of 2019, according to World Health Organization data released in July. The fall in overall childhood vaccinations in 2021 was the biggest in 30 years, with at least 25mn infants missing out on routine immunisations.
“Polio is becoming a big threat again and the risk is that, if it spreads across too many geographies, it will be impossible to eradicate,” says Dr Zulfi Bhutta, chair of child global health at Hospital for Sick Children, Toronto.
He co-ordinated the publication this month of a global declaration on polio signed by more than 1,000 scientists, urging support for Gpei. “You cannot do science on thin air — you have to have the resources,” says Bhutta, who cited vaccine hesitancy as a key challenge to overcome.
Rockland, a county about 30 miles north-west of New York City, has become a case study in how poor vaccination rates can leave communities vulnerable to outbreaks.
About 325,000 people live in the commuter town, which is home to a large and growing Orthodox Jewish community that has become the target of increasingly vocal anti-vaccine campaigners.
Childhood vaccination rates for two-year-olds in the county average 60 per cent and drop to 37 per cent in some postcode areas. This is significantly below the 80 per cent level that the WHO says is required to provide herd immunity for polio and the 95 per cent level required for measles.
“This is not a religious issue,” says Dr Patricia Ruppert, Rockland’s health commissioner. “It is an issue that, in some insular communities, we are seeing misinformation being propagated over a number of years, unfortunately — so it is a lot to tackle and is a great challenge.” The “politicising” of vaccine efforts during the pandemic has deterred a lot of people from getting inoculated, she says.
Authorities have established pop-up vaccination clinics, stepped up education campaigns, and told medical centres to be on alert for polio — which can present as flu-like symptoms, or often no symptoms at all.
“There is not really any treatment for polio so it’s prevention that is key in this case,” says Ruppert, adding that 7,000 polio vaccines have been administered in Rockland since July 21.
Wastewater surveillance is a crucial tool that has tracked the spread of the polio virus to several counties — and linked the Rockland case to the UK and Israel. Rockland authorities have started auditing schools to ensure they are complying with a legal requirement that all pupils are vaccinated. This was introduced in 2019 following a measles outbreak, which made hundreds of children unwell and also centred on the Orthodox Jewish community.
In developing countries, particularly Pakistan and Afghanistan where wild polio remains endemic, the challenge of vaccine hesitancy is compounded by poor infrastructure, conflicts, and climate-related disasters.
But Dr Jay Wenger, who leads a polio programme at the Bill & Melinda Gates Foundation, says Gpei could achieve its eradication goal if the $4.8bn it is seeking is raised.
The recent development and roll out of a new oral polio vaccine called nOPV2, which is more stable and less likely to cause VDP outbreaks, had provided a new tool for prevention, he says.
More funding could complete the vaccination rollout in Pakistan and Afghanistan, mop up outbreaks of VDP and eliminate the risk of the virus spreading. Wenger says: “The longer we go with virus still floating around somewhere, the longer we have this risk of it popping into places that are under-vaccinated and causing problems.”
Comments