How Africa fought the pandemic — and what coronavirus has taught the world

Roula Khalaf, Editor of the FT, selects her favourite stories in this weekly newsletter.
This story is part of a major Financial Times series Coronavirus: could the world have been spared?, investigating the global response to the crisis and whether the disaster could have been averted.
HIGH ALERT
The threat from the north

In a deserted wing of the African Union complex in Addis Ababa, John Nkengasong was hunched over a desk peering at numbers. It was early evening and almost everyone had gone home, disappearing into the dusty air of the Ethiopian capital. The large, drab room was one of several occupied by the Africa Centres for Disease Control and Prevention, a pan-African public health agency charged with bolstering health systems across the vast continent of 54 nations. Africa CDC was only three years old and Mr Nkengasong was its first director.
The date was February 18 2020.
Four days earlier, Egypt had reported Africa’s first case of coronavirus when a Chinese national tested positive after flying into Cairo. So far, no further infections had been confirmed. But Mr Nkengasong, a virologist who had been working in public health for three decades, knew what was coming.
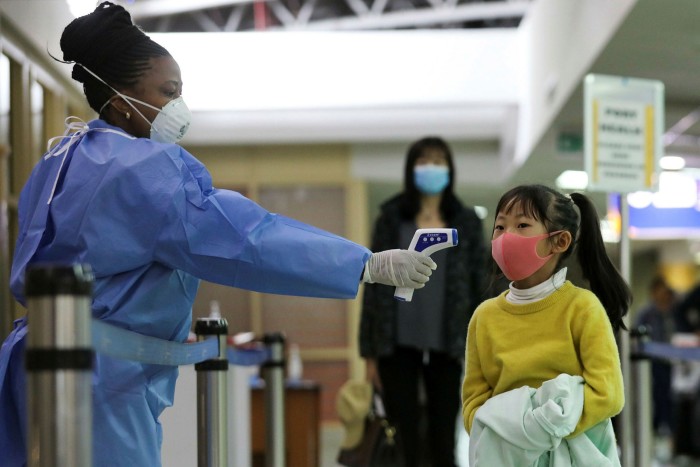
Although Europe had barely woken up to the threat of Covid-19, Africa was on high alert. At Bole International Airport in Addis Ababa, where half a dozen planes from China rumbled in each day, masked staff were collecting passenger information and checking temperatures.
The same was happening across the continent. People with fevers were tested for Covid-19, but all came up negative. The first case in sub-Saharan Africa would not be confirmed until February 28, 10 days later, when an Italian businessman developed symptoms after travelling to Lagos, Nigeria’s vast commercial capital.
Genomic analysis would later reveal that almost all infections brought into Africa came not from China but from Europe, what Mr Nkengasong calls an “amphibious attack”. It is a reversal of the normal patterns of infectious disease in which Africa is so often the epicentre. This time, the threat was coming from the north. Looking back at the initial months of the pandemic, when it was overwhelming sophisticated health systems in Italy, Spain and Britain, Mr Nkengasong recalls the shock he felt. “We watched with total fright and awe what was happening in Europe. We knew we had no chance if that happened here on that scale.”
Apart from a handful of countries, such as South Africa and Egypt, there were virtually no intensive care units in a continent of 1.3bn people, although sophisticated equipment would not be the key to managing the pandemic, even in rich countries. Still, a grim factoid was doing the rounds: South Sudan, Africa’s most recent state and among its most troubled, had fewer ventilators (four) than vice-presidents (five).
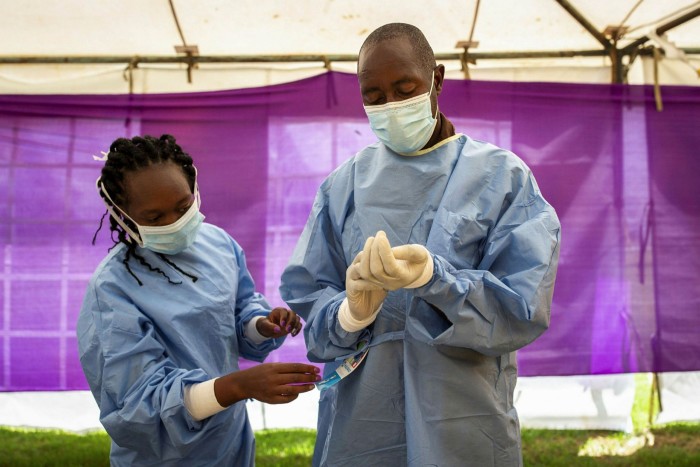
Early intervention would be vital. Mr Nkengasong sent someone to Germany to bring back 10,000 emergency test kits. Meanwhile, the Louis Pasteur Institute in Dakar, Senegal, a world-class facility run by Amadou Sall, a Senegalese virologist, started training technicians to test for the new disease. By the end of February, 42 countries had the capacity to test for Covid-19. Just a few weeks before, there were none.
Mr Nkengasong speaks in measured tones, but his sense of urgency is palpable. He has spent much of his career battling human immunodeficiency virus, which causes Aids, a disease that had only recently emerged when he began his medical studies in the mid-1980s. HIV has since infected 75m people worldwide and killed 32m, the majority in Africa. Like HIV, which spread to humans from monkeys, coronavirus jumped from an animal, in this case a bat. The working theory is that Sars-Cov-2, the virus that causes Covid-19, probably made the leap to people via a mammal, possibly a pangolin butchered at a wet market in the Chinese city of Wuhan.
Mr Nkengasong watched with alarm as this new virus infiltrated every Chinese province. Beijing restricted the movement of 60m people. “That’s like the whole population of South Africa or Kenya,” he says, eyes widening. “Once this thing gets out of control, it will be very, very hard for our health systems to handle.”
In almost every respect, Africa is at a disadvantage compared with richer continents. Apart from one. Africans know all too much about infectious diseases. While the virus sent Europeans and Americans into panic, many Africans shrugged. “Here comes another one,” said Laurie Garrett, author of the 1994 book The Coming Plague. Scattered around the continent, there are people of Mr Nkengasong’s calibre, veterans of hard-knock battles against endemic diseases such as malaria, tuberculosis and cholera, and more recently emerging ones such as Lassa fever and HIV/Aids. “I can pick up the phone and speak to any one of them,” said Mr Nkengasong.
Before a single confirmed case of Covid-19 in sub-Saharan Africa, Mr Nkengasong convened an emergency two-day meeting of health ministers in Addis Ababa. “I have never been this serious in my life,” he said. “They came from Egypt, Morocco, Nigeria, South Africa. Everybody was there.” Not long after, Cyril Ramaphosa, president of South Africa and chairman of the African Union, began organising weekly video conferences to co-ordinate Africa’s response. “I don’t know any continent that rallied that quickly,” recalls Mr Nkengasong.
Inevitably, the virus pierced Africa’s hastily erected defences, spreading to almost 40 countries by March 20. But numbers were relatively low and many countries mounted an aggressive effort to snuff out new infections.
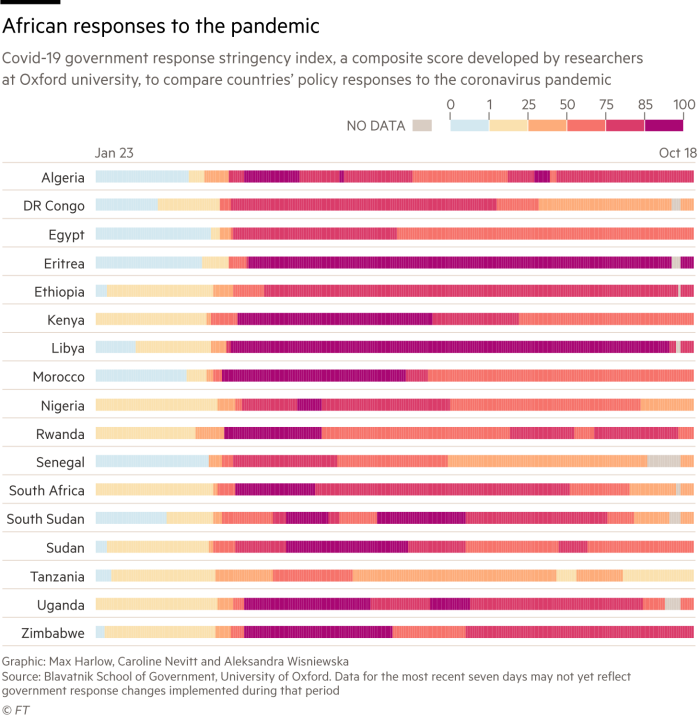
Rwanda, in central Africa, was one of the most aggressive. On January 31, it cancelled flights from China. A week after the first case slipped through the net in March, it suspended international flights altogether, closed its borders and told people to stay indoors. “This is what any country should have done,” says Agnes Binagwaho, vice-chancellor of Rwanda’s University of Global Health Equity. “We didn’t do this because we are rich. We did it because we are organised.” South Africa also took bold steps. On March 23, before a single Covid-19 death, President Ramaphosa announced a three-week lockdown, one of the strictest in the world. All but essential workers were ordered to stay at home and sales of alcohol were banned.
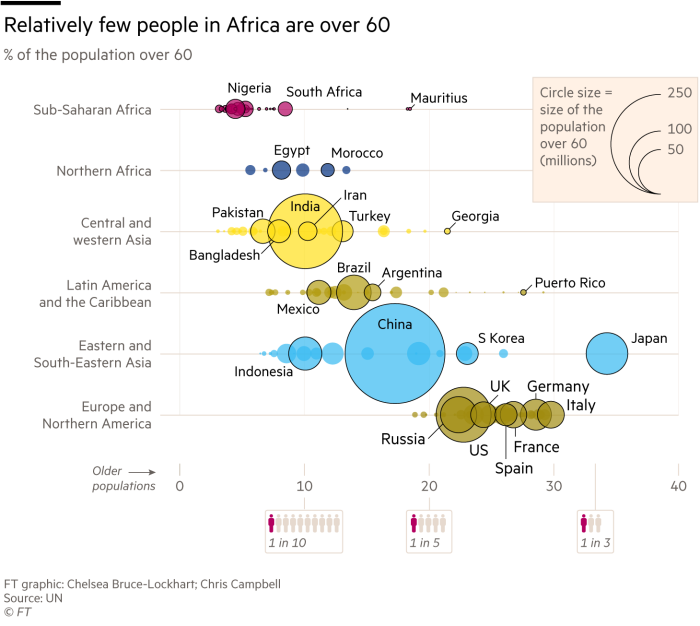
Not all countries could do likewise. Indeed, there was an argument that western-style lockdowns might do more harm than good. Poor people had to eat. And insisting they stayed in crowded informal settlements was hardly a recipe for social distancing. Some warned that lockdowns were an overreaction. After all, Africa has a very young population, with a median age of 19.4, about half that of Europe. There is little obesity. If societies shut down, then vital programmes — including vaccination campaigns and maternal healthcare — could stop, causing more damage than Covid-19 itself.
Governments had to weigh up the risks. Most stopped short of full lockdown, but erred on the side of caution. Countries from Senegal to Uganda closed schools, churches mosques, and banned mass gatherings. Ethiopia tried a low-tech response. According to Arkebe Oqubay, special adviser to the prime minister, by late-May authorities had surveyed 40m of the country’s 110m people, checking temperatures and travel history. “This is not a disease you fight by ventilators or intensive care units,” he said. “The only way we can play and win is if we focus on prevention.”
Still, there were agonising choices. Kenya imposed a dusk-to-dawn curfew. At one point, more people had been shot for defying it than had died of Covid-19. Kennedy Odede, who helped distribute soap to slum-dwellers in Nairobi, said: “They are telling me we better die from coronavirus than die from hunger.”
Despite the hardship, people took the health threat seriously. Conductors on Nairobi’s crowded matatu minibuses sprayed customers’ hands before they climbed on board. In west Africa, dustbin-sized “Veronica Buckets”, used in the Ebola outbreak (2013-16), appeared outside offices and shops so people could wash their hands under a little tap. Safaricom, the telecoms operator that pioneered mobile money, waived fees for many transactions on its M-Pesa service to help discourage the use of cash.
Not all governments took Covid-19 seriously. In Tanzania, President John Magufuli, known as “The Bulldozer” for his uncompromising style, denied it posed a threat. He urged Tanzanians to work and gather as normal. The funerals of many who died were carried out at night.

Even when governments took decisive action, the virus spread. Deaths were concentrated at the extreme north of the continent, in Morocco, Egypt and Algeria, and in the extreme south, in South Africa, where almost half of all deaths occurred. By July, some hospitals were overwhelmed. New infections were hitting 12,000 a day and by September, South Africa would register more than 16,000 deaths. But by then the country was moving into the southern hemisphere’s summer and the epidemic was easing. New infections fell dramatically.
South Africa may have been harder hit than others because its population is older or because there are more people with diabetes and heart disease. The rest of the continent has so far avoided the worst of the coronavirus storm. By October, Africa, which makes up 17 per cent of the global population, had recorded just 3.5 per cent of Covid-19 deaths.
The low fatalities, even if they underestimate the true numbers, could not be attributed to policy alone. It looked increasingly as if other factors, including pre-exposure to related viruses, might have made people less vulnerable to Covid-19, although scientists said it was too early to tell. Besides, the pandemic might have further to run. Still, policy played a vital role. “Never before had Africa managed such a response,” says Peter Piot, director of the London School of Hygiene and Tropical Medicine. “Remarkably, they acted even before they had a problem.”
GLOBAL RESPONSE
Too early — and too late

India acted early too. On March 24, after registering barely 550 infections and about 10 deaths, Narendra Modi, the prime minister, made a dramatic announcement. The country’s 1.4bn people, he said, should not leave their homes. If India did not get the next 21 days right, he warned, it risked being set back 21 years.
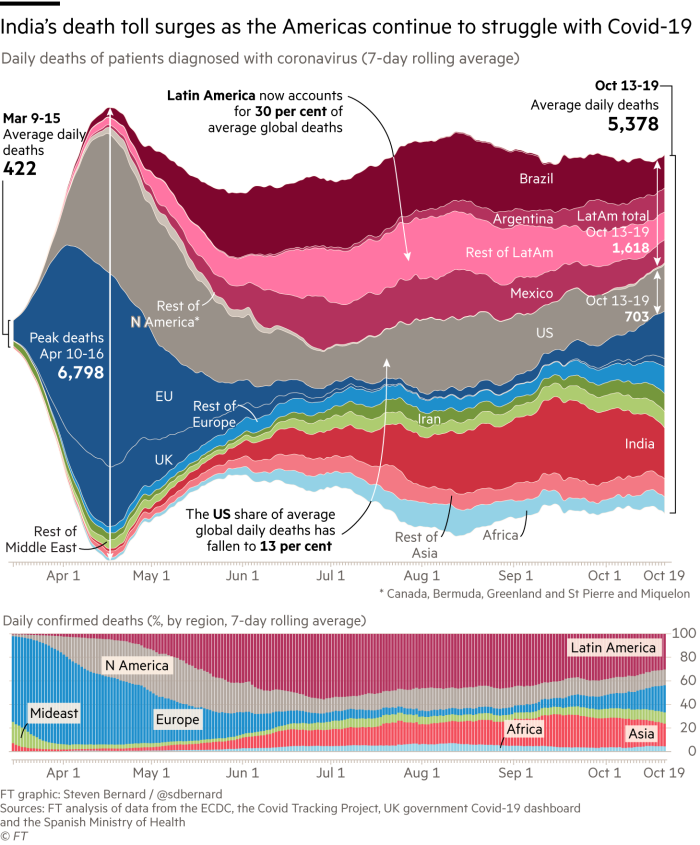
It did not get it right. By sending tens of millions of migrant workers scrabbling to get home with just a few hours’ notice, the lockdown may actually have helped spread the virus from cities such as Delhi, Mumbai and Pune to every corner of the subcontinent. By October, India had recorded almost 100,000 deaths, the third-highest after the US and Brazil. Confirmed infections shot past 6m. Serological tests suggested at least 100m people might be infected.
“The lockdown did not help much in terms of reducing transmission, but it bought us time,” says Bhramar Mukherjee, professor of biostatistics at the University of Michigan. Yet, in the absence of robust public health infrastructure, including testing capacity, the epidemic slipped out of control.
After weeks of stringent lockdown, the government abruptly changed tack, telling Indians they must learn to live with coronavirus. Many were desperate to work, whatever the consequences. “It is very hard to convey a public health message to someone who is not sure where their next meal is coming from,” says Shahid Jameel, chief executive of the Wellcome Trust/DBT Alliance, a biomedical charity. The government, he says, made things worse by massaging numbers. It marshalled an apparently low fatality rate as evidence that government policies were working. “There’s a narrative based on cherry-picking of data, which has made people tired and complacent.”
Prof Mukherjee says that people who had taken to dangling masks like necklaces instead of wearing them properly were either in denial or had resigned themselves to the virus’s inevitable spread.

Worse affected still has been Latin America. In ascending order of deaths, Bolivia, Ecuador, Chile, Argentina, Colombia, Peru, Mexico and Brazil have all been pummelled by the virus. Countries have been hit whether they acted early, like Chile and Peru, or left matters to fate like Brazil whose president, Jair Bolsonaro, mocked the virus as “sniffles”. About half of all Covid-19 fatalities have occurred in the Americas. Brazil alone has recorded more than 155,000 deaths, making it the worst-hit nation after the US.
The country of 210m people has a strong record combating HIV and experience with emerging diseases, such as Zika, which struck in 2015. But Margareth Dalcolmo, a pulmonologist with the Rio de Janeiro-based Fiocruz, a state-funded research institute, says the medical community’s strategy has been undermined by the government from the start. “We have insisted that social distancing is an important arm of our response. But unfortunately, the government was completely against us.”
Rather than amplifying a science-based message, she says, Mr Bolsonaro’s government has sown confusion. Although up to 30 per cent of people may have already been exposed in big cities like Rio de Janeiro and São Paulo, she forecasts the virus still has two years to run.
PARADOX OF PROGRESS
The lessons of Covid-19

In assessing whether the world could have been spared the Covid-19 pandemic, it is helpful to consider the question in two parts. First, how prepared were societies for the almost inevitable emergence of a disease against which humans had zero immunity? And second, how did they handle it once it actually struck?
Those fighting infectious diseases had for decades been warning about the risks of a pandemic. It was dangerous to pigeonhole pathogens as “tropical diseases” in an era of jet travel when microbes could hitch a ride to anywhere on earth, they say. “I think that, in the mindset of the west, it was always a threat that was for the developing world, especially for Africa,” says Mr Nkengasong. “The characterisation of ‘tropical medicine’ meant ‘these people in Africa or the tropics’, which were considered a ‘museum of diseases’.”
In 1981, Richard Krause, former director of the National Institute of Allergy and Infectious Diseases, told the US Congress: “Plagues are as certain as death and taxes.” Jonathan Mann, a pioneer of HIV research in the 1980s, wrote that Aids was trying to teach humanity “that a health problem in any part of the world can rapidly become a health problem to many or all”. The world desperately needed a worldwide “early-warning system” to detect the eruption of new diseases. Without it, he warned, “we are essentially defenceless”.
Coronavirus: could the world have been spared?

The coronavirus pandemic has killed more than 1m people across the globe. But could it have been averted? A unique FT investigation examines what went wrong — and right — as Covid-19 spread across the world
Part 1: China and Covid-19: What went wrong in Wuhan
Part 2: The global crisis — in data
Part 3: Why coronavirus exposed Europe's weaknesses
Part 4: Will coronavirus break the UK?
Part 5: How New York’s missteps let Covid-19 overwhelm the US
Part 6: How Africa fought the pandemic — and what coronavirus has taught the world
Major outbreaks of Ebola in Africa from 1976, of severe acute respiratory disease, or Sars, in China in 2003, and of swine flu in Mexico in 2009, proved that microbes remained a potent force.
Ebola showed how even the most “exotic” and frightening disease can spread, first to west Africa, where it killed 11,300 people, and from there as far afield as Dallas and Glasgow, admittedly in tiny numbers. Sars, too, infiltrated the US, New Zealand and South Africa, infecting a total of 8,096 people and killing 774. The H1N1 strain of swine flu moved from Mexico to the US before infecting people worldwide with a lab-confirmed death toll of 18,449 and probable fatalities many multiples of that.
Yet the false sense of security in the west persisted. Humans had made remarkable progress against the microbial threat through advances in public health. The widespread use of antibiotics by the 1940s only added to the growing sense of infallibility. Smallpox was eliminated in the 1970s. By 2001, in high-income nations, only 6 per cent of deaths were caused by infectious disease. It was tempting to think that sickness spread by bacteria, viruses, parasites and protozoa could be squeezed out altogether.
This was a false conclusion. The proportion of people dying from infectious disease may have been falling, but the emergence of new ones — spread from animals — was gaining speed. Paul Hunter, professor in medicine at the University of East Anglia, says 335 new infectious diseases emerged in humans between 1940 and 2004.
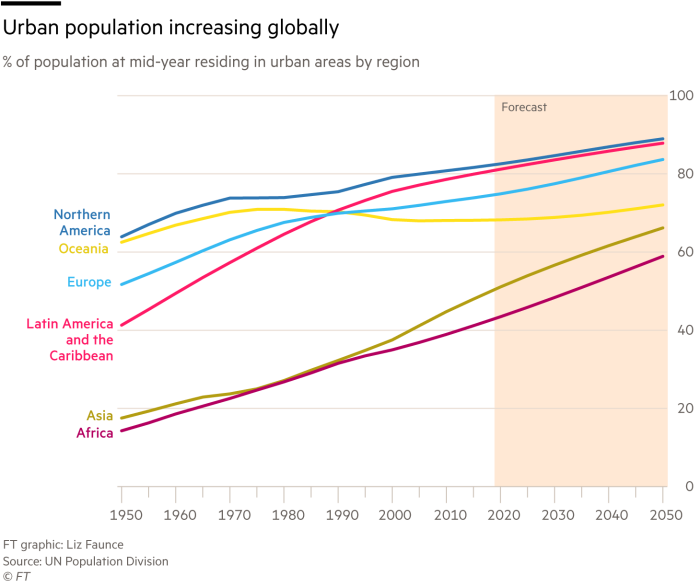
The persistence of the microbial menace owed partly to the paradox of progress. Advances in nutrition and medicine allowed the human population to explode from 1.6bn in 1900 to 7.8bn today. People have crowded into ever-larger conurbations. As they encroached on rainforests, they and their domesticated animals came into closer contact with wildlife. And between 1970 and 2018, according to the World Bank, air passenger numbers rose from 310m to 4.2bn, bringing people together from every corner of the planet. It was a microbe’s paradise.
Added to this was the trade in wild animals, which transported exotic species to markets in China, south-east Asia and elsewhere. If isolated communities eating bushmeat contract a new disease, it tends to die out. But if animals are transported to densely populated cities, a new disease can rapidly spread. “If this trade had been stopped, then [Covid-19] almost certainly would not have happened,” says Prof Hunter.
There was another reason humans were ill-prepared for a pandemic they should have seen coming, says William Haseltine, an American scientist and businessman who has specialised in HIV/Aids and pioneered the use of genomics for drug discovery. That was a failure to direct science at the most potent threats.
Outside HIV, where pressure groups successfully lobbied for funding, the response to new diseases has been lacklustre, he says. He cites Sars, which like Covid-19 is caused by a coronavirus found in bats. Public funding initially flowed into finding treatments. “There was tremendous effort put in by researchers all over the world during the early phases of Sars. But when, after about nine months, Sars sort of faded away, they pulled the plug.”
The same thing happened with Middle East respiratory syndrome, or Mers, another coronavirus, this one from camels. After an outbreak of Mers in Saudi Arabia in 2012, there was a flurry of research. “Then the plug got pulled again,” says Mr Haseltine. “It was virtually impossible to get funding even though we were clearly warned,” he says. No drugs that might have treated, or prevented, coronavirus diseases completed clinical trials.
Mr Haseltine mentions research into protease inhibitors of the sort used against HIV to block an enzyme that viruses use to multiply. “That drug works equally well in tissue culture experiments and animal experiments against Sars-Cov-1 and Sars-Cov-2. Had we taken that and other drugs to a human development stage . . . almost nobody needs to have died in China. And nobody needs to have died in the US,” he said. “Because that drug, if given prophylactically to exposed people, would almost certainly have stopped the [Covid-19] infection in its tracks.”
Yet the big money, especially that spent by pharmaceutical companies, has gone into heart disease, cancer, kidney disease, diabetes and degenerative illnesses such as Alzheimer’s. These conditions have two things in common. They are non-infectious and they affect people with money. “People often talk about a boom and bust cycle of our investments in preparing for pandemic threats,” says Thomas Bollyky, director of the global health programme at the Council on Foreign Relations. “But it’s really just been bust.”
Trudie Lang, director of the Global Health Network at the University of Oxford’s Nuffield Department of Medicine, says there are two big obstacles to funding infectious disease research. On the technical side, trials can only run once an outbreak has occurred. Then there is a narrow window before the disease disappears. That is what developers of vaccines against coronavirus initially found: it was hard to prove a vaccine’s efficacy when the virus was not circulating.
In addition, said Prof Lang, most grants for research go to teams led by superstar investigators at famous universities, usually in rich western countries. That squeezes out equally deserving research in low and middle-income countries. “That’s the 90:10 gap,” she said. “Ninety per cent of research benefits people in just 10 per cent of the world.”

Mr Jameel at Wellcome Trust/DBT Alliance says: “Big pharma has stopped investing in infectious disease. You take an anti-bacterial or an antiviral only until you clear the infection. But once you start on a statin or anti-diabetes medicine, you have to take it for life. Big pharma is investing in chronic disease because that is where the money is.”
Noam Chomsky, the linguist and political activist, puts it more starkly, calling the failure to prepare science to fight coronavirus “a colossal market failure”. For pharmaceutical companies, he said in a recent interview, “making new body creams is more profitable than finding a vaccine that will protect people from total destruction”.
Ms Garrett said there had been a subtle shift from a view of health as a public good to something that was essentially individual. In Betrayal of Trust: The Collapse of Global Public Health, she wrote that the way to prevent the “coming plague” of her previous book went beyond a “technological quick fix”. Instead, it needed what she called a global public health infrastructure of surveillance and prevention, a dam that could “hold back the river of microbes and pathogens”.

But public health is under assault. There has been a backlash in some rich countries against vaccines, the ultimate public good. Before Boris Johnson, the UK’s prime minister, fell ill with Covid-19 himself, he had voiced opposition to a sugar tax, which health experts argued was a weapon in the war on obesity but which many in Britain thought an unnecessary intrusion of the “nanny state”.
In poor countries, public health is even more vital, but even more neglected. In 2017, Nigeria, Africa’s most populous country, spent $74 per capita on health, less than one-hundredth of the $8,000 spent by Norway. “The greatest error we’ve made is to take the public out of public health,” says Oyewale Tomori, a fellow of the Academy of Science of Nigeria.
If health is increasingly a question of individual responsibility, then linked to that, say experts, is a shift towards technology as the principal weapon against disease. Both US president Donald Trump and Mr Bolsonaro have favoured the miracle cure over the hard slog of pandemic response. Prof Hunter says the problem with pre-emptive public health is that it is invisible. “Nobody notices if you stop an outbreak. They only notice if you don’t.”
Covid-19, then, burst upon a world that had neglected the required tools to fight pandemics: infectious diseases research and investment in public health systems. Even as word of a new coronavirus in China began to trickle through to Europe and America, authorities remained strangely unalarmed.
That may, in part, have been due to the initial suppression of information in China. “For the first critical three weeks there was not the transparency that would have been required to contain the emerging infection,” says Mr Bollyky. “China does bear some of the responsibility, though by no means all, for what happened.”
Beijing’s secrecy highlighted the World Health Organization’s lack of authority to compel individual nations to divulge information. “We need to be less reliant on the compliance and transparency of nation states around emerging infections,” says Mr Bollyky. “From the WHO perspective, I’m largely sympathetic to the challenges they face. But I do think they hurt themselves a bit by praising China’s early performance. That undermined their credibility with other states.”
Still, by mid-January, it ought to have been obvious that the virus spiralling out of Wuhan had the makings of a global pandemic. Some countries, notably in north and south-east Asia, took the threat seriously. That was partly because they had experienced the devastating impact, not least economic, of Sars. Others — among them the US, Brazil and to some extent the UK — were less alert to the danger.
“The countries that moved aggressively in using proven measures to suppress the spread of emerging infections — testing, identifying cases, contact tracing, isolation and quarantine — enjoyed great success,” says Mr Bollyky. “Even countries that were seen as not having a great deal of resources, like Vietnam, used tried-and-tested measures that date back ultimately to the 14th century.”

Mr Haseltine argues that, to combat a pandemic, states need at least two of three qualities: leadership, governance and public solidarity. The US, he argues, has none of the three in sufficient quantities and has suffered the consequences. “By governance, I mean, a national public health system that can execute and implement policy on a national level. China has it, most European countries have it. We don’t. When Trump says ‘it’s not my problem’, he’s actually right. The same kind of chaotic organisation, lack of central administration [and] lack of capability to create policy and execute policy that currently exists for testing, exists for vaccine distribution,” says Mr Haseltine. “And you can expect the same result.”
“I think countries that have done well have listened to science and countries that have done badly have not listened to science,” says Wellcome’s Mr Jameel. “China was very authoritarian, but they listened to everything science told them.” Still, even China was caught off guard by an event that was utterly predictable.
Governments, just like individuals, are bad at planning for “Black Swan” events, says Prof Mukherjee, the biostatistician. “You have to play the long game in public health. It would have been much better to have financed contact tracing for 100 years than to have spent trillions of dollars on economic stimuli," she says, referring to the massive government intervention after Covid-19 crippled economies around the world.
“We always live in reaction mode,” says Mr Jameel. “We don’t live in pre-emptive mode.”
The kind of foresight required does not come easily. But it is not as if we have not been warned.
Join the conversation
How has the pandemic been handled where you live? What has gone right or wrong for you during this time? Do you work in a sector that was hit hard by lockdowns? Or have you managed to adapt your life positively? Share your experiences in the comments below.

Comments